Pregnant women often undergo a slew of tests during their pregnancy, including ultrasounds, urine and blood tests. Some women may remember downing a sickly-sweet drink as part of the glucose challenge test and the Glucose Tolerance Test, which test for gestational diabetes (GDM). But what is this form of diabetes, and what are the risk factors, possible outcomes and treatments? Cayman Health investigates.
What is gestational diabetes?
“Gestational diabetes is the term used for describing diabetes first diagnosed during pregnancy,” explains Endocrinologist and Internist Dr. Diane Hislop-Chestnut of Palm Road Medical Limited.
GDM occurs during pregnancy and usually disappears after giving birth. It generally occurs around week 24 of pregnancy but can occur at any time.
GDM occurs when the mother’s body cannot make and use all the insulin it needs during pregnancy. Insulin is a hormone made by your pancreas that acts like a key to let blood sugar into the cells in your body for use as energy. Without enough insulin, glucose builds up in the blood, leading to hyperglycemia (high blood sugar levels).
Diabetes UK cites studies that put U.K. GDM rates as occurring in 5 percent of all pregnancies, while a 2014 analysis by CDC stated that GDM prevalence is as high as 9.2 percent in the U.S. The true prevalence of gestational diabetes is hard to establish however, and data for Cayman specifically is hard to obtain.
“Prevalence [of GDM] has been increasing over time, possibly due to increases in maternal age and weight,” says Dr. Hislop-Chestnut.
Associated problems
Most women with gestational diabetes deliver healthy babies, however uncontrolled GDM can bring potential issues, to both mother and baby.
GDM can lead to larger babies due to the increased levels of glucose crossing the placenta, and therefore increased chance of labor difficulties, inducing or caesarean section. GDM also increases the chance of too much amniotic fluid in the womb, which can cause premature labor or delivery problems. Risk of premature birth is also increased, and well as the baby having low blood sugar levels or jaundice. Risk of stillbirth is also increased although rare.
GDM also increases the mother’s risk of high blood pressure and preeclampsia, as well as future development of type 2 diabetes.
Risk factors
Women are at increased risk of gestational diabetes if they are over 25 years old; if their BMI is over 30; if they have prediabetes; if they previously had a baby born weighing 10lbs or more; if gestational diabetes occurred in a previous pregnancy; if the mother’s parents or siblings have diabetes; or if family origins are south Asian, Chinese, African-Caribbean or Middle Eastern.
Testing
GDM does not usually cause symptoms, but may do if the mother’s blood sugar level gets too high – known as hyperglycemia. Symptoms may include increased thirst, urinating more frequently, dry mouth and tiredness.
The likelihood of problems associated with GDM can be reduced if it is detected and well managed.
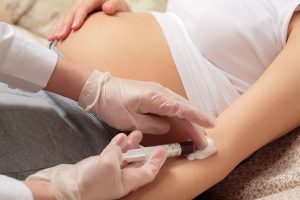 An initial glucose challenge test will assess the mother’s risk for GDM. The mother must drink a syrupy glucose solution and have blood drawn one hour later to measure blood sugar level. A blood sugar level below 140 milligrams per deciliter (mg/dL) is usually considered normal on a glucose challenge test, although this may vary by clinic. If the mother has a higher than normal blood sugar level, she will need a glucose tolerance test to establish a GDM diagnosis.
An initial glucose challenge test will assess the mother’s risk for GDM. The mother must drink a syrupy glucose solution and have blood drawn one hour later to measure blood sugar level. A blood sugar level below 140 milligrams per deciliter (mg/dL) is usually considered normal on a glucose challenge test, although this may vary by clinic. If the mother has a higher than normal blood sugar level, she will need a glucose tolerance test to establish a GDM diagnosis.
For a follow-up glucose tolerance test the mother must fast overnight, then have her blood sugar level measured. She must then drink another sweet solution — this one containing a higher concentration of glucose — and her blood sugar level will be checked every hour for two to three hours. If at least two of the blood sugar readings are higher than normal, she may be diagnosed with gestational diabetes.
Treatments
“Usually diet control and exercise will treat most patients,” says Dr. Hislop-Chestnut. “Those who are not able to reach the blood glucose goals will need insulin.”
Blood sugar testing kits are available to monitor blood sugar levels, and the mother’s doctor or a dietitian may be able to help with healthy eating plans and appropriate levels of physical activity.
As for post-birth risks, Dr. Hislop-Chestnut explains that “women who have had GDM are at higher risk of developing type 2 diabetes in the future.” Worryingly the CDC says that about 50 percent of women with GDM go on to develop type 2 diabetes.
“[Women who have had GDM] should be tested 4 -12 weeks after delivery and screened at least every three years thereafter,” advises Dr. Hislop-Chestnut, in an effort to diagnose and treat possible type 2 diabetes quickly.
Prevention
 If overweight, losing weight and increasing physical activity before pregnancy may reduce the risk of it occurring. Remember weight loss is not advised while pregnant.
If overweight, losing weight and increasing physical activity before pregnancy may reduce the risk of it occurring. Remember weight loss is not advised while pregnant.
Women should also talk to their doctors about recommended weight gain during pregnancy to reduce their risk of GDM.







